The Problem of PPE Provisions — What’s The Solution?
It’s hard to escape the endless news cycle on the lack of PPE for frontline healthcare staff in hospitals and social care settings across the country. While supply chains are part of the problem, there are also challenges with the PPE itself as explained in Part One of our NHS blog series, challenges that largely revolve around face masks.
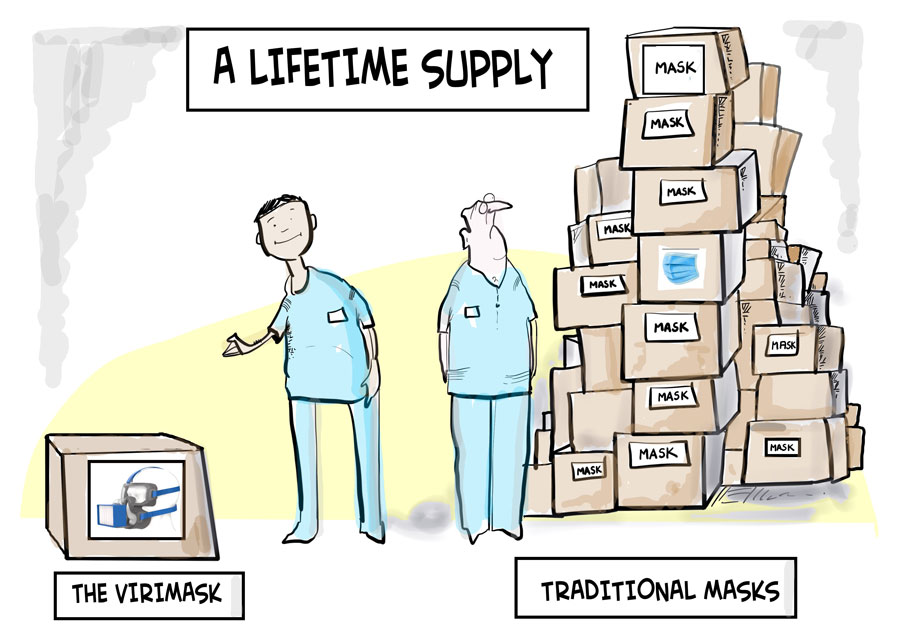
Single-use face masks for COVID-19 protection put greater strain on supply chains and budgets as hundreds of thousands of masks are used and disposed of daily. Then there are issues of effectiveness, ease of use and comfort.
Whether its an N95 face mask or FFP3 face mask, it requires proper fitting to be truly effective. Fittings can take up to an hour. Even with correct fitting, limited sizing options make all kinds of PPE, from face masks to gowns and gloves, difficult to work in, especially for female staff with smaller faces and statures.
As for comfort, staff often endure 8–12-hour shifts wearing a complete set of PPE — gown, gloves, face mask and eye protection. An uncomfortable face mask only adds to the physical strain they are under, with many left with pressure marks on their faces after a long day or night at work.
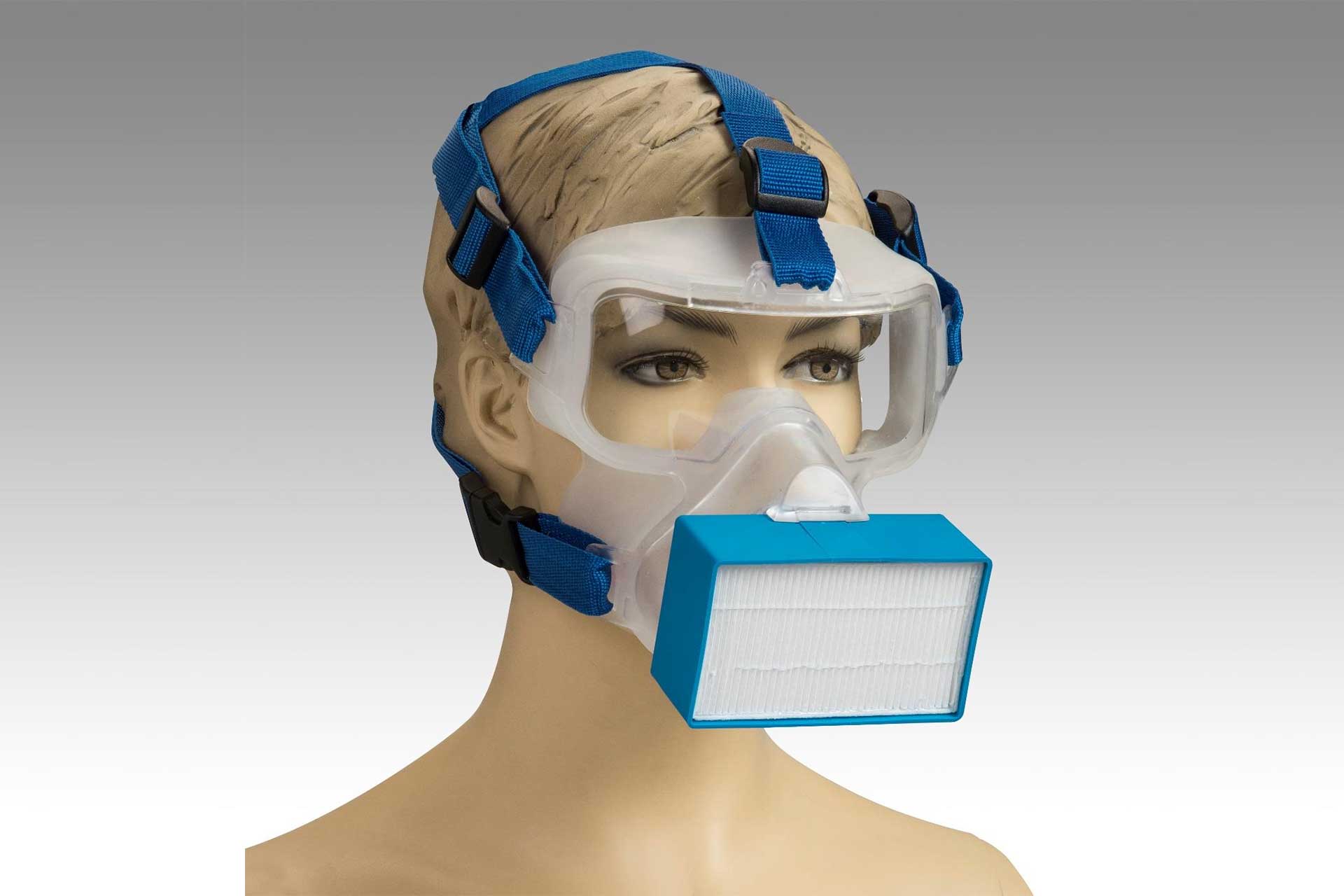
So what is the solution? The NHS has turned to industry to help solve the PPE problem, not only by boosting supply but also through innovation. We explore how a new coronavirus face mask, the Virimask, can help in Part Two of our NHS blog series. We reveal how it can provide an effective alternative to N95 face masks, while also offering eye protection, a more comfortable fit and avoiding the waste of single-use face masks.
Countries world-over continue to face PPE problems but solutions, such as the Virimask, are changing the state of play so we’ll all be better prepared for future outbreaks.